
Our Research

Research Focus
Technology With Purpose: Advancing Rehabilitation Through Innovation and Values
Our research is organised around a central question: how do we get the most promising rehabilitation technologies to the people who need them, reliably, affordably, and equitably?
Answering that question requires more than engineering. It requires understanding clinical workflows, healthcare economics, patient experience, environmental impact, and the complex realities of implementation within resource-constrained systems like the NHS. Our research operates across these dimensions, using Rehabilitation 4.0 technologies as the means and Rehabilitation 5.0 principles as the framework for decisions about what to build, how, and for whom.
A history of Rehabilitation Revolutions
1
 (1)
(1)
Rehabilitation 1.0: Mechanisation
Mechanical aids, passive devices, pulley systems, and basic orthoses. The formalisation of physical rehabilitation as a discipline, driven largely by the needs of injured soldiers during and after the World Wars.
2
 (2)
(2)
Rehabilitation 2.0: Electrification
Electrical stimulation, powered prosthetics and orthoses, electromechanical devices. Standardised clinical protocols and the growth of physiotherapy and occupational therapy as professions.
3
 (3)
(3)
Rehabilitation 3.0: Computerisation
Computer-controlled devices, early rehabilitation robotics, computer-based assessment, digital outcome measurement, and the first use of virtual reality in therapeutic settings.
4
 (4)
(4)
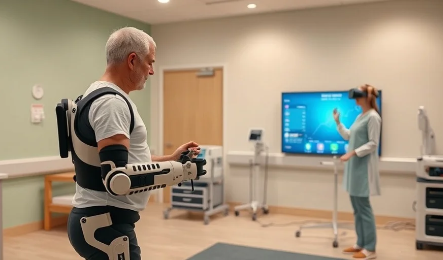
Rehabilitation 4.0: Intelligent, Connected Systems
AI and machine learning, IoT-enabled wearable sensors, adaptive robotics, brain-computer interfaces, serious games, telerehabilitation, and data-driven personalisation of therapy.
5

Rehabilitation 5.0: Human-Centred, Sustainable, Equitable
Co-design with patients and clinicians, environmentally sustainable technology, equitable access across populations, resilient systems that strengthen rather than strain the healthcare workforce, and meaningful human-technology collaboration.
Our Approach
We focus on technologies that have demonstrated promise in controlled settings but face barriers to real-world adoption. Our role is to close that gap, developing the methods, evidence, and practical solutions needed to move interventions from laboratory to clinic to home.
Two decades of experience with what works, what fails, and why shapes every aspect of this work. We pursue innovations that are scientifically exciting but also implementable, sustainable, and scalable.
Rehabilitation 4.0: The Technological Foundation
Rehabilitation 4.0 draws on Industry 4.0 principles (intelligent systems, connectivity, data-driven decision-making) applied to the challenge of motor recovery. These are the core technology domains we work across:
Adaptive robotic systems delivering personalised, real-time assistance for upper and lower limb motor recovery.
BCIs that decode neural signals to drive rehabilitation devices and promote neuroplastic recovery.
Interpretable machine learning that predicts recovery, optimises treatment, and adapts interventions in real time.
VR and AR environments that deliver engaging, adaptive practice to drive motor learning in clinic and at home.
Wearable and multi-modal sensors that quantify movement and track recovery beyond the clinic.
Pairing rehabilitation technologies with electrical and transcranial stimulation to maximise neuroplastic change.
Remote-supervised therapy systems that extend safe, effective rehabilitation into the home.
Rehabilitation 5.0: The Guiding Philosophy
Rehabilitation 4.0 addresses what technology can do. Rehabilitation 5.0 addresses what technology should do, and for whom. These principles shape how we set priorities, design systems, and evaluate outcomes:
We co-design rehabilitation technologies with patients, carers, and clinicians, embedding lived experience from the outset.
We design rehabilitation technologies for longevity, efficiency, and minimal waste across their full lifecycle.
Technologies that support rather than burden clinicians, working reliably across varied settings and changing circumstances.
We design with underserved populations in mind, so rehabilitation technology narrows rather than widens health inequalities.
Translation: From Evidence to Impact
We view research as complete when a technology is in routine clinical use, not when it demonstrates efficacy in controlled trials. This translational commitment means we address questions that extend beyond traditional research: cost-effectiveness within NHS funding models, integration with clinical workflows, staff training requirements, and strategies for scaling across healthcare systems.
Our position within the UK healthcare landscape gives us direct access to these challenges. We work with NHS trusts, understand constrained budgets and stretched workforces, and design our research to generate evidence that matters to healthcare decision-makers.

The Stroke Recovery Garden at Chapel Allerton Hospital
- Wellcome Trust Library. Physical Therapy at Bath War Hospital. Watercolour by E. Horton (no. 44761i). Available at: https://search.wellcomelibrary.org/iii/encore/record/C__Rb1202573. Accessed 27 February 2026.
- MIT Museum - Liberty Mutual Insurance Co. supported the development of the Boston Arm as a way of getting amputees off disability and back on the job. Available at: https://spectrum.ieee.org/ingestible-electronics. Accessed 27 February 2026.
- Sivan, M., Gallagher, J., Makower, S. et al. Home-based Computer Assisted Arm Rehabilitation (hCAAR) robotic device for upper limb exercise after stroke: results of a feasibility study in home setting. J NeuroEngineering Rehabil 11, 163 (2014). https://doi.org/10.1186/1743-0003-11-163
- Afridi A, Obaid S, Raheel N, Rathore FA. Integrating Artificial Intelligence in Stroke Rehabilitation: Current Trends and Future Directions; A mini review. Available at: https://yesilscience.com/integrating-artificial-intelligence-in-stroke-rehabilitation-current-trends-and-future-directions-a-mini-review/. Accessed 27 February 2026.

